Heart Failure-Lifespan And Quality Of Life Is Worst Than Cancer If Left Undiagnosed And Untreated
Dr Wong Teck Wee
Consultant Cardiologist
iHeal Medical Centre (www.ihealmedical.com)
Level 7 & 8, Annexe Block, Menara IGB, Mid Valley City,
Kuala Lumpur, Malaysia
What Is Heart Failure?
Doctors may describe heart failure as an enlarged, swollen or weak heart. Sometimes it may be referred to as congestive heart failure. Thats because some patients have fluid accumulation or congestion primarily in the lungs. Heart failure is NOT a heart attack. A heart attack usually results from blockage in the blood vessels that cut off the supply of blood to the heart muscle. Unlike a heart attack, heart failure is a chronic progressive weakening of the heart muscle. It develops when the heart's muscle becomes weakened after it is injured and loses its ability to pump enough blood to supply the vital organs. Those remaining healthy parts of the heart get more and more stretched out and weaker, almost like a stretched out balloon or rubber band.
Alarming Statistics
Ageing population and improved treatment of cardiovascular disease, in particular of acute heart attacks, kept more people alive, however at the cost of weakened heart muscle. In Western world average prevalence of heart failure is 2-2.5%, increasing to >10% in octogenarians. Framingham Heart Study showed for those after 40 years old their lifetime risk of heart failure is 20%. Heart failure is the most frequent cause of hospitalization in people age 65 and older. Health care costs of heart failure are high because of frequent and often lengthy hospitalizations, particularly in the elderly heart failure patient with more co-morbidity. In US, hospitalization costs account for 60-70% of all heart failure expenditure and is twice the amount spent for all forms of cancer combined.
Heart failure is a malignant disease
Heart failure does not occur in isolation. Most patients have other diseases as well.
The European Heart Failure Survey in patients > 70 years indicated that 27% had diabetes mellitus, 16% chronic kidney failure, 32% lung diseases and that approximately 20% were anemic. Patients with HF have a worse quality of life than those with other chronic diseases including bronchitis/emphysema, kidney failure and arthritis. End stage heart failure patients will suffer from breathlessness at rest. In these patients, walking to the toilet is like running a marathon. Heart failure has a worse prognosis than most cancers. Up to 40% of patients die within one year of diagnosis. Sudden deaths are 6-9 times more common than in general population. 5-year survival is 25% in men and 38% in women (Framingham study), but in breast cancer 5-year survival is 70%.
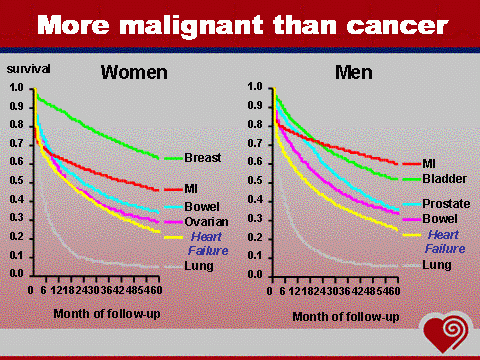
Fig 1 Stewart S, MacIntyre K, Hole DJ, Capewell S, McMurray JJV. Eur J Heart Fail
2001; 3: 31522.
What are the symptoms of heart failure?
Many people are not aware they have heart failure because the most common symptoms are often confused with normal signs of aging and many patients may be asymptomatic. Also, people often try to avoid symptoms by making lifestyle changes, such as taking the elevator instead of the stairs. Some of the warning signs of heart failure are fatigue, giddiness, shortness of breath, cough, loss of appetite, scrotal and leg swelling. Since the blood is not being squeezed out of the heart effectively, it tends to pool up or dam in the lungs and into the rest of the body which produces shortness of breath, intestinal and leg swelling. Some people even wake up suddenly from sleep feeling the need to catch their breath. Patients may not be able to lie flat and prefer to sleep on elevated pillows.
What are the causes of heart failure?
Heart failure is the final outcome of any injury to the heart. Risk factors include: heart attack, high blood pressure, damage to heart valves, heart muscle viral infection and genetic predisposition. Muscle damage and scarring caused by a heart attack is the most common cause of heart failure. Persistent uncontrolled high blood pressure and cardiac arrhythmia (irregular heartbeat) also increases heart failure risk. Advanced age also adds to the potential impact of heart failure outcome.
How Do I Know if I Have Heart Failure?
Only your doctor can tell if you have heart failure. When you visit your doctor, he will take your medical history and examine for signs of heart failure. One of most important diagnostic tools for heart failure is called an echocardiogram or ECHO for short. It is a painless and non-invasive procedure using ultrasound that allows your doctor to see how vigorously the heart is contracting. The ejection fraction is a measurement of how well your heart is pumping. Another test is an electrocardiogram or ECG. A chest X-ray will show an enlarged heart size. Some centres may offer a simple blood test called BNP (B type natriuretic peptide) to screen for heart failure.
Is There a Cure For Heart Failure?
While there is currently no known cure for heart failure, early diagnosis and proper treatments may help patients live longer by slowing the progression of disease and keep them out of the hospital. A critical part of heart failure therapy involves taking medication. Experts now recommend a multi-drug treatment regimen as part of the standard of care to treat heart failure. Some medications are prescribed to control symptoms caused by the congestion, while others are used to slow down the progression of heart failure. Diuretics, sometimes called water pills, help remove extra fluid in the body and reduce swelling in the legs and ankles. It is important to remember that even when the congestion goes away, the heart failure is still there. Thats why it is so important to treat not just the symptoms, but the underlying disease.
Long term outcome of heart failure
It is important to remember that heart failure does not mean that the heart suddenly stopped working or that you are about to die. Heart failure is not a death sentence. With the right treatment, salt and fluid restriction, you can live comfortably with heart failure. In fact, millions of people are living with heart failure right now. If you do have heart failure, its important for you to play an active role in managing your condition. Youll want to keep in regular touch with your doctor. Also, youll need to watch your diet, particularly your salt intake. Eating too much salt causes the body to retain too much water, making the fluid buildup even worse. If you notice weight gain for three days continuously, youre probably retaining too much water. Its important to see your cardiologist as soon as possible to avoid a life threatening admission to the hospital. On the other hand, your heart and circulation can benefit from regular exercise when you are not breathless, but be sure to talk to your doctor before starting any exercise program.
Click here to return to main news update page
Please stay tuned for our next congress and article update!
Please visit our congress website at: www.healthyageingcongress.com
or like our facebook page at: www.facebook.com/healthyageing
For other enquiries please email us at: info@dynamicmerit.com
2011. All Rights Reserved. Dynamic Merit Sdn Bhd.
 Malaysian Healthy Ageing Society
Malaysian Healthy Ageing Society
